Frustrated by your child’s eczema? Here are some things you should know
If your child suffers from eczema, you know that it can be a challenge to manage the condition. It can often feel like no matter what you do, you can’t seem to get it under control. Despite your best efforts, you’re unable to rescue your child from the itching, the scratching, the rashes and the sleepless nights that ensue. Your child is very literally wearing the evidence of this struggle for the world to see. It’s a terrible feeling, really- that you’re powerless to help your child- but that’s how eczema often makes us feel because it just keeps coming back.
Some good news about eczema
Eczema treatment is moving in a new direction. The medicines themselves aren’t new, but experts have realized that perhaps shifting the focus of our treatment will produce better outcomes.New studies have shown the importance of what’s called “skin-directed management,” meaning we focus more on treating the skin itself than we have in the past. Previously, there’s been a lot of importance placed on the relationship between food allergies and eczema. Parents have been directed to get their children allergy tested and then restrict certain foods with the idea that the food allergy is the ultimate cause of the child’s skin problems. There’s more and more evidence, though, that food allergies might not be the ultimate cause of eczema for a lot of people. While it’s true that people who suffer from food allergies are often the same people who suffer from eczema, correlation doesn’t equal causation. In other words, just because both exist in the same patient, it doesn’t mean one caused the other. It could simply be that what makes it more likely for someone to have one condition also makes it more likely that someone has the other, too.
Experts are beginning to place less emphasis on withholding certain foods from eczema sufferers as a primary treatment. New research has brought forth the idea that rather than an allergic reaction, eczema may be a problem with the skin itself. The primary purpose of our skin is to provide a barrier against the outside world- to keep the good things in our body and the harmful things out. In eczema sufferers, the skin barrier may be less effective at keeping moisture in and keeping irritants and allergens out. Treating the skin itself may be the way to address the real problem.
How should I manage my child’s eczema?
There are four main components to skin-directed management.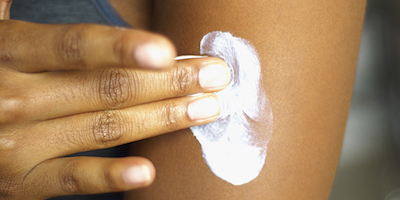 Maintenance skin care. This is the toughest one to manage. It requires consistency and a fierce commitment to doing the same things day in and day out, but the hard work is worth it. The goal is to repair and maintain the skin so it can function the way it is supposed to, and this is accomplished through skin hydration. Moisturizers should be applied at least once daily (often after a lukewarm bath to retain the moisture from the bath) over the entire body, not just the eczema-prone areas. Use a moisturizer that doesn’t have additives, fragrances or “extra stuff” in it that could be irritating to the skin. Typically, a cream or ointment is best. Ointments (such as petroleum jelly or brand names such as Aquaphor) are often more moisturizing, but they can leave an oily feeling or oily stains on fabric. Lotions are not as effective at moisturizing, but creams are somewhere in the middle of those two.
Maintenance skin care. This is the toughest one to manage. It requires consistency and a fierce commitment to doing the same things day in and day out, but the hard work is worth it. The goal is to repair and maintain the skin so it can function the way it is supposed to, and this is accomplished through skin hydration. Moisturizers should be applied at least once daily (often after a lukewarm bath to retain the moisture from the bath) over the entire body, not just the eczema-prone areas. Use a moisturizer that doesn’t have additives, fragrances or “extra stuff” in it that could be irritating to the skin. Typically, a cream or ointment is best. Ointments (such as petroleum jelly or brand names such as Aquaphor) are often more moisturizing, but they can leave an oily feeling or oily stains on fabric. Lotions are not as effective at moisturizing, but creams are somewhere in the middle of those two.
The important thing to remember is to be consistent, every single day, even when the symptoms aren’t visible.
Steroid creams or ointments. When a flare-up occurs (when the skin becomes red and inflamed), moisturizing alone can’t solve the problem. You’ll need a steroid cream or ointment (what your doctor might call a topical anti-inflammatory medication). This may be as simple as using over-the-counter hydrocortisone cream or your doctor may give you a prescription. Use this cream once or twice a day for one or two weeks until the skin is no longer irritated, as directed by your doctor.
Address the itching. If your child has severe itching (especially if it is keeping them awake at night), talk to your doctor about how you can help control the itching. An oral antihistamine (such as Benadryl) might help. Talk with your doctor about it first, though, because antihistamines aren’t recommended for young children without a doctor’s supervision. Remember that the consistent use of moisturizers will help resolve the itching as well.
Here are a few questions that might be helpful to you as you begin this conversation with your pediatrician:
Questions to ask your doctor
- How often should my child have a bath? The answer to this question is often very specific to the child and their symptoms. Sometimes daily baths are best, sometimes every other day is optimal. Talk it over with your pediatrician and come up with a plan.
- Do I need to have a prescription for a topical steroid or should I use an over-the-counter medicine? Also, be sure you’re clear on exactly when and how to use the steroid cream.
- Do you recommend the use of an oral antihistamine (Benadryl) to help with itching?
- Which type of moisturizer do you recommend? Do you suggest a cream or ointment, a particular brand name?
- Should I change my laundry detergent, shampoos, soaps?







