Why does my baby's skin look yellow?
Jaundice is one of those medical terms that you may have heard on occasion, but can’t quite pinpoint what it means exactly. However, if you’re the parent (or soon-to-be parent) of a newborn, it will be helpful for you to become familiar with this common issue affecting babies soon after birth.
What is jaundice?
The term “jaundice” refers to the yellowish color of the skin (or whites of the eyes) seen in many newborns. It’s one of the things your baby’s doctor will assess after birth and before sending your baby home from the hospital. This yellow tint to the baby’s skin is seen in approximately 60 percent of newborns, and it is generally mild and temporary. However, it is something that must be closely monitored within the first week of baby’s life, because bigger problems can arise in some infants if not handled appropriately.
The yellowish color comes from a build-up of bilirubin in the body. Sometimes you might hear your doctor refer to jaundice as “hyperbilirubinemia” which, in essence, means too much bilirubin in the blood. Bilirubin is the yellow/orange sludge that is left over after the body’s normal process of breaking down older red blood cells, and it is supposed to be removed by the liver then excreted in the stool.
The liver of a newborn is immature, however, and sometimes cannot process the bilirubin quickly enough, resulting in an increase of bilirubin in the body and a yellowish coloring of the skin. For most babies, this is a normal process that occurs within the first week of life and will resolve over a few weeks as their liver gets better at removing bilirubin. Others may need some medical intervention to bring their bilirubin levels back down.
Things to keep in mind soon after baby’s birth
Babies who are breastfed tend to experience jaundice more often than others, especially if they are having trouble breastfeeding. Since bilirubin is sent out of the body through feces, it makes sense that an infant who isn’t eating or pooping much isn’t able to get the excess bilirubin cleared as quickly. Be sure to nurse your new baby 8 to 12 times a day within the first few days of life to ensure proper nutrition, keep bilirubin levels down and maintain your milk supply. If you have any problems nursing, be sure to ask your doctor or nurse for a lactation consultant who will help you work through any breastfeeding issues you may encounter.
Contact a lactation consultant here.
A newborn’s bilirubin levels are usually highest 3 to 5 days after birth. This is often after mother and baby have been released from the hospital, so even if your baby didn’t experience jaundice while in the hospital, it can still become an issue at home. If baby is released from the hospital before he is 72 hours old, it is extremely important that you see your pediatrician within two days after returning home from the hospital.
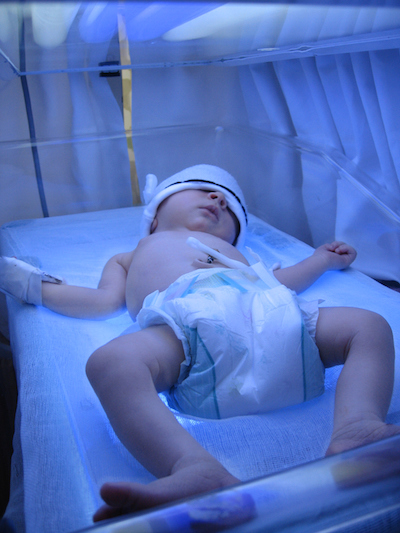
Keep in mind that most of the time jaundice needs no treatment. Often, your doctor will simply monitor baby’s bilirubin levels as you continue to feed baby normally and monitor his stool, and the issue will resolve over time. Sometimes, though, babies need a little extra help, and they will be placed under bright lights called phototherapy. (You may hear hospital staff refer to these purple fluorescent lights as “bili lights.”) This light helps convert bilirubin to another form where it is easily removed from the body through natural processes.
Infants who are born before 37 weeks of gestation, have a sibling who experienced hyperbilirubinemia or experience jaundice within the first 24 hours after birth are more likely than others to need medical intervention.
It is critical for your pediatrician (both in the hospital and outside the hospital) to monitor your baby’s bilirubin levels within the first week of life. Although a high bilirubin level is most often a mild issue that resolves on its own, in rare cases bilirubin can increase to dangerous levels that may cause brain damage.
If you notice the skin or whites of your baby’s eyes looking yellow, call your pediatrician’s office. If your baby appears yellow and seems to be difficult to wake, fussy or has trouble feeding, follow up with your doctor right away.







